One of the most frequently used proverbs in the Healthcare sector comes from a 4,000-year-old Chinese text; “Superior doctors prevent disease.” Swap out the word ‘doctor’ for ‘healthcare system’ and you get a succinct definition of what modern healthcare systems aspire to: prevention rather than costly remedial treatment.
But, as every healthcare professional will tell you, achieving a seamless continuum from consultation to treatment to monitoring conditions or the taking of medication and follow-up care, is extremely difficult. The many pressures on healthcare professionals at all levels – from GP surgeries to hospitals and clinics and community care providers – are hampering the provision of joined-up care.
Healthcare under pressure
That results in ‘care gaps’ across both the private and public healthcare sectors. And those gaps make it more difficult to deal with the pressures that come from an ageing population, rising numbers of chronic long-term conditions, and an increasing demand on healthcare systems. Of course, all those issues are impacted by wider social and environmental challenges, political uncertainty, a ‘cost of living crisis,’ the effects of climate change, and often severe shortages of healthcare professionals and ancillary workers.
All those elements undermine achieving a holistic continuum of care and means that healthcare systems find it hard to focus on prevention rather than cure.
Is technology the answer?
Digital leaders in the healthcare sector are constantly looking to improve how they can use data to triage patients faster and more accurately, create a seamless data-driven pathway from treatment to support, medication, and follow-up, and apply digital solutions to share data securely and in a timely fashion so that both prevention and treatment are patient-focused. All with cost benefits to whoever is paying for the care – the state, the insurer, or the patient themselves.
Technology is a key part of the answer. But it’s not a panacea. AI (and the rapid rise of headline-grabbing techs like ChatGPT etc.), improved connectivity via 5G, genetic engineering, robotics and automation all have a role to play in improving the patient experience. Together they can enable healthcare professionals to work more efficiently (while relieving the stress of skills gaps and long hours), but the most essential element in any technological fix is – the data.
“Superior data prevents disease.”
OK, so data isn’t going to cure anyone directly, but it’s the key to fulfilling the promise of the Continuum of Care. Data isn’t just ones and zeros that can be read by a computer; data is a flow of information that, when it gets stuck or lost, inhibits the ability of professionals and patients alike to take the right actions to achieve well-being. Data oils the machine. It illuminates both patient and professional pathways. There are many metaphors I could use, but you get the point.
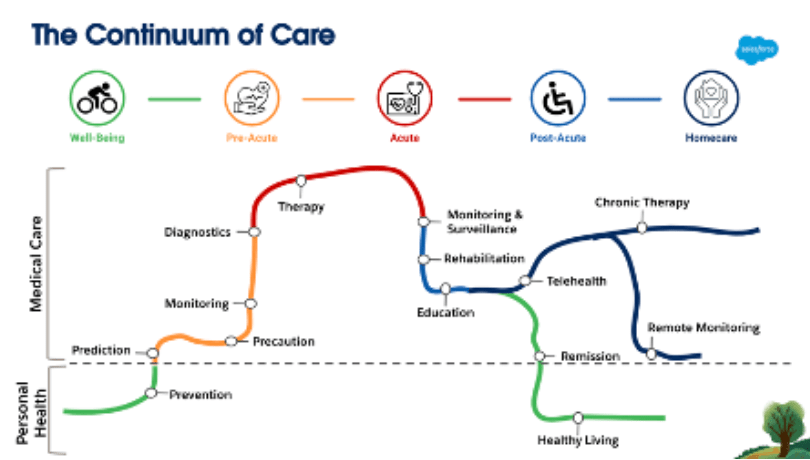
The whole point of a ‘continuum’ is to enable elements which are related to each other but different from each other to work in harmony. So, that encompasses every element of healthcare, from prevention to consultation to treatment, follow-up, and medication. And back again. It doesn’t matter if the elements are entirely public or private, funded by taxes or insurance, the continuum must be patient-centric. And data is what makes it all work seamlessly.
Data – it should be about people; patients and professionals who help them
Salesforce is known for its CRM expertise, and I’m the first to admit that customer-relationship management comes across as something that retailers or marketing people use. Talking about CRM in a healthcare context can cause some people to become uneasy. It doesn’t sound serious enough; it’s all about using data to send out marketing materials or special offers on detergents. Yes, it is. But it’s so much more than that.
In fact, when you think about it, ALL data interactions between healthcare organisations, as well as the people they serve or the people who for or with them, need some kind of CRM system. The better the system, the better the flow of data. And when data flows smoothly, as I’ve stressed before, the more efficiently a continuum of contact as well as care works.
So, the point is to transcend the cliches about CRM and even drop the acronym. Let’s call it PRM – patient relationship management, or people relationship management. Any word that describes the patients, the professionals, and all the care workers across the healthcare spectrum. The right kind of PRM means that boundaries between public and private, prevention and treatment, follow-up, and medication, can be overcome so that at any point on the continuum you get a complete picture of each relationship. That’s how you achieve meaningful action which benefits all stakeholders.
Salesforce actually has a deep and varied involvement in the healthcare sector. That’s a fact that surprises many. We’re constantly working to provide the flow of data that can close the care gaps which hinder the successful operation of the continuum of care.
Power Efficiency in Healthcare
Reduce costs while providing excellent care, thanks to a single 360-degree view of every patient — made possible with a connected CRM solution.












